
The respiratory tract of asthmatic patients is very sensitive. When stimulated by allergens, strong reactions will occur, and the airway will become narrow, resulting in dyspnea.
We can intuitively understand the changes of children’s airway when asthma attacks through the figure.
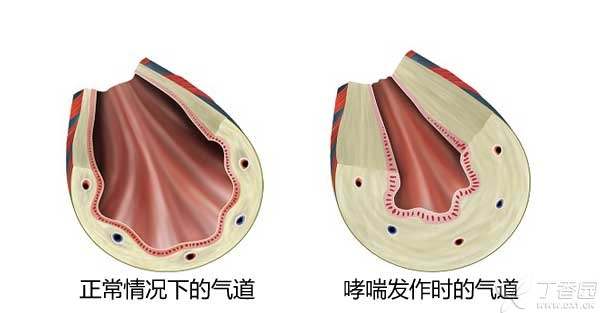
Because children’s airway development is not mature, asthma poses a greater threat to children. If children’s asthma is not treated properly, the acute attack of asthma may be fatal.
Will the child have asthma?
Asthma is very [cunning], especially in young children. It is likely to be confused with acute or chronic bronchitis, pneumonia and chronic cough.
Therefore, parents should be alert to whether the child suffers from asthma when the child has the following conditions.
- Repeated attacks of bronchitis, pneumonia or lower respiratory tract infection; Cough for more than 3 weeks; Other possible respiratory tract infections have been ruled out.
If the child suffers from asthma, TA may say something like [my chest is uncomfortable] or [I always cough].
Symptoms of asthma may worsen at night, so pay attention to whether children cough or wake up from cough during sleep at night. Crying, laughing, shouting or other intense emotional reactions, as well as stress, may all induce cough or wheezing.
Do you want to take the child to the doctor?
Although children’s asthma cannot be cured, the symptoms may continue into adulthood. However, through standardized treatment, asthma can be controlled and its damage to children’s lung development can be prevented.
If you suspect your child has asthma, please take the child to see a doctor in time. Early treatment can not only effectively control the general symptoms of asthma, but also prevent the acute attack of asthma.
Please see a doctor as soon as possible when you find that your child has the following conditions:
-
Persistent cough, which intensifies during activities;
-
Exhalation is more laborious, sometimes accompanied by a slight whistle;
-
Shortness of breath or shortness of breath
-
Under the age of months, breathing ≥ 60 times/min; 2 ~ 12 months old, breathing ≥ 50 times/min; 1 to 5 years old, breathing ≥ 40 times/minute. The number of breaths can be counted by observing the ups and downs of the child’s thorax, and one breath and one inhalation are recorded as one breath.
-
The child reported chest discomfort.
-
Repeated attacks of bronchitis or pneumonia.
Please go to the emergency department immediately in case of any of the following situations:
-
Children need to stop to breathe when they speak normally.
-
Breathing mode is obviously different from usual.
-
Inhalation nasal alar incitement is obvious;
-
During inhalation and exhalation, depressions can be seen under the neck, under the thorax and between the ribs.

What preparations do you need to make before seeing a doctor?
Before seeing a doctor, please do the following work:
-
Write down all the symptoms your child has, whether it appears to be related to asthma or not.
-
Write down when the symptoms affect the child most, for example, when the symptoms tend to worsen during the day; A specific season; Children are exposed to cold air, pollen or other possible incentives; When doing sports or playing.
-
Write down key personal information, including whether the child’s recent life has changed or there is pressure.
-
Write down the drugs and dietary supplements your child has recently taken.
Home Care Suggestions
Reducing children’s exposure to asthma stimulators can reduce the probability of asthma attacks, which can be achieved through the following measures:
-
Ensure indoor air is clean. Check the air conditioner every year, clean it regularly and replace the filter screen. At the same time, install the filter screen on the ventilation equipment.
-
Clean animal hair. If children are allergic to animal hair, the best way is to avoid them. Regular cleaning of pets can reduce the drop of their hair in the environment.
-
Use air conditioner or air purifier. Air conditioner helps to remove pollen in the room. At the same time, it can reduce the humidity of the air in the room and reduce dust particles. If there is no air conditioner, please close the window as much as possible during the pollen season.
-
Reduce dust. Regular change of bedding can reduce dust, because dust can aggravate symptoms at night. Use floors instead of carpets as much as possible, especially in children’s rooms.
-
Clean regularly, at least once a week, and pay attention to let children wear masks to avoid dust stimulation.
-
Moderately humidify the air. If the child’s symptoms will worsen in dry and cold environment, please reduce the exposure of the child to cold air.
-
Rational use of drugs and active treatment of any disease related to asthma.
-
Control the child’s weight, ensure that the child has sufficient activities, and do not stop eating because of choking.
The prevention of asthma is very simple and includes three aspects:
-
Avoid asthma stimulation sources as much as possible, which is the best way to prevent asthma, paying special attention to stay away from second-hand smoke environment;
-
Encourage children to take more activities and exercise lung function;
-
When you need medical treatment, go in time and don’t carry it, because asthma changes.
Is how [under control of asthma]?
The goal of asthma treatment is to control asthma. Good control has the following goals:
-
Mild or asymptomatic;
-
The number of acute attacks of asthma is few or no.
-
There will be no restriction on activities;
-
Rapid remission drugs (such as salbutamol) are used less;
-
The reaction to the drug is good, with little or no side effects.
In fact, world famous star Beckham and swimmer Phelps are all asthmatic patients. Through regular drug therapy and exercise programs, they can also run on the green field and gallop through the waves.
Editor: Zhang Jingyuan
Author: Er Meow Jushi
This article is reprinted by Clove Garden authorized by the author.
